We help healthcare providers and billing companies streamline their medical billing operations using a powerful blend of Artificial Intelligence (AI) and Robotic Process Automation (RPA).
Our mission is to eliminate manual errors, reduce claim denials, and accelerate payment cycles — enabling healthcare professionals to focus on patient care, not paperwork.

Extract patient demographics, diagnosis codes, and payer details from EHRs, PDFs, and scanned forms using AI-based OCR.
AI agents validate CPT, ICD, and HCPCS codes before claim submission.
RPA bots file claims across multiple payer portals and update status in real time.
AI models identify denial reasons, suggest corrections, and re-initiate resubmissions automatically.
Real-time tracking of claims, payments, and denial trends through a single dashboard.

Collect structured and unstructured billing data from multiple sources.

AI agents validate and standardize claim information.
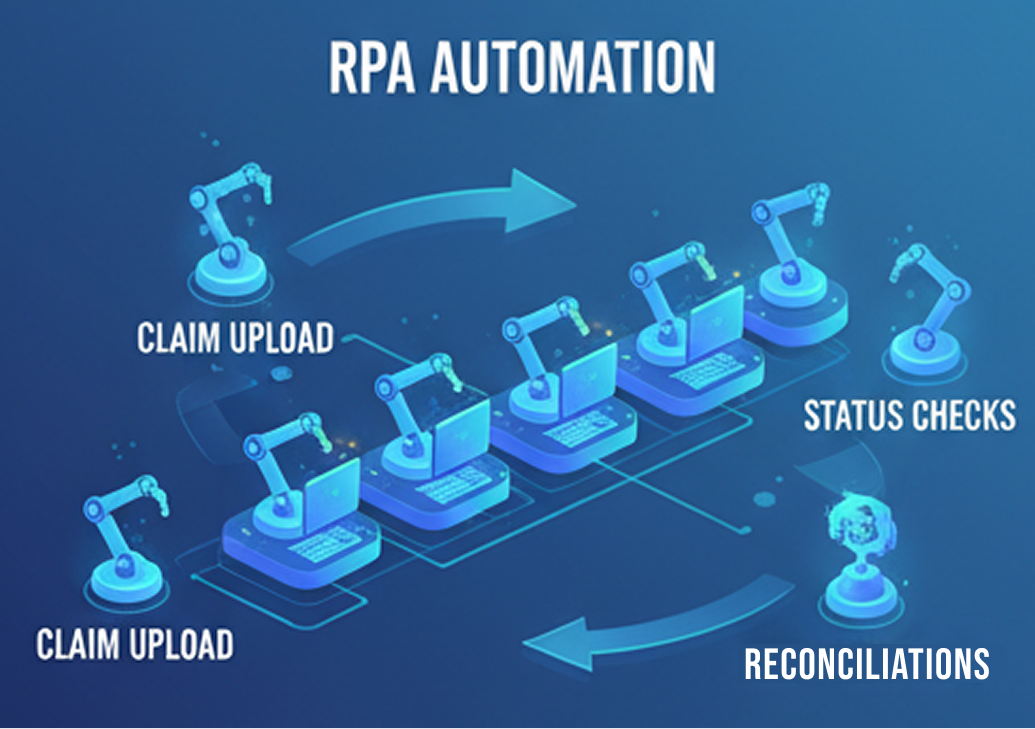
RPA bots handle repetitive workflows such as claim uploads, status checks, and reconciliations.

Dashboard provides visual analytics and automatic alerts for pending or rejected claims.

Whether your billing team handles hundreds or thousands of claims, our solution scales to fit your workflow.
Reduction in Manual Processing
Accuracy in Data Extraction and Coding
Faster Claim Reimbursements
Claim Tracking & Analytics
with Existing EHR/ERP Systems
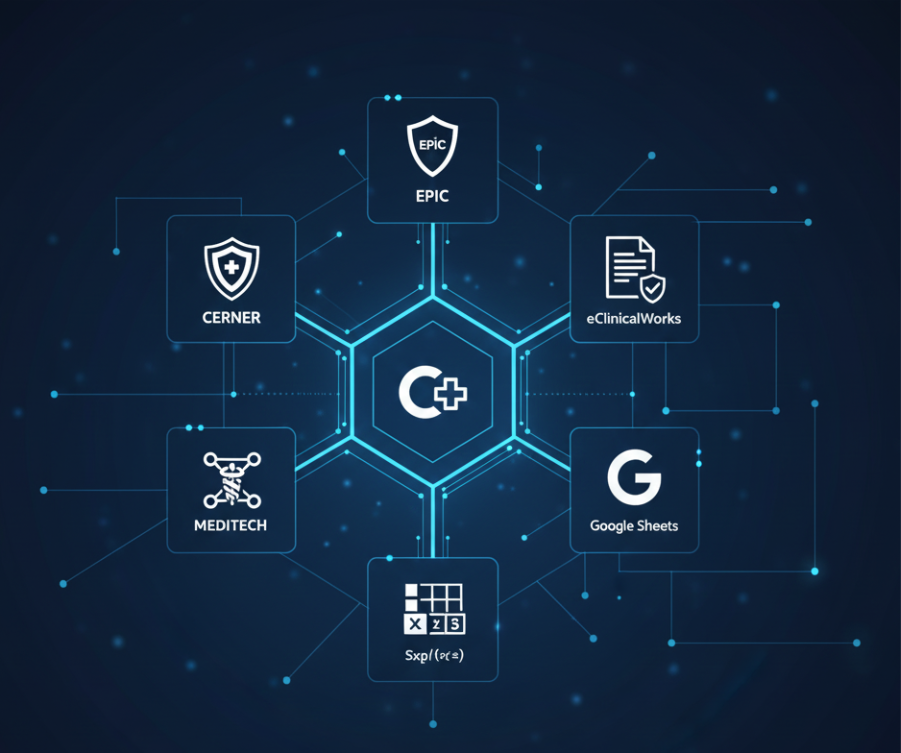
We ensure end-to-end data security and regulatory compliance with HIPAA, GDPR, and ISO 27001 standards.
All sensitive healthcare data remains encrypted and securely processed.
Easily integrates with: